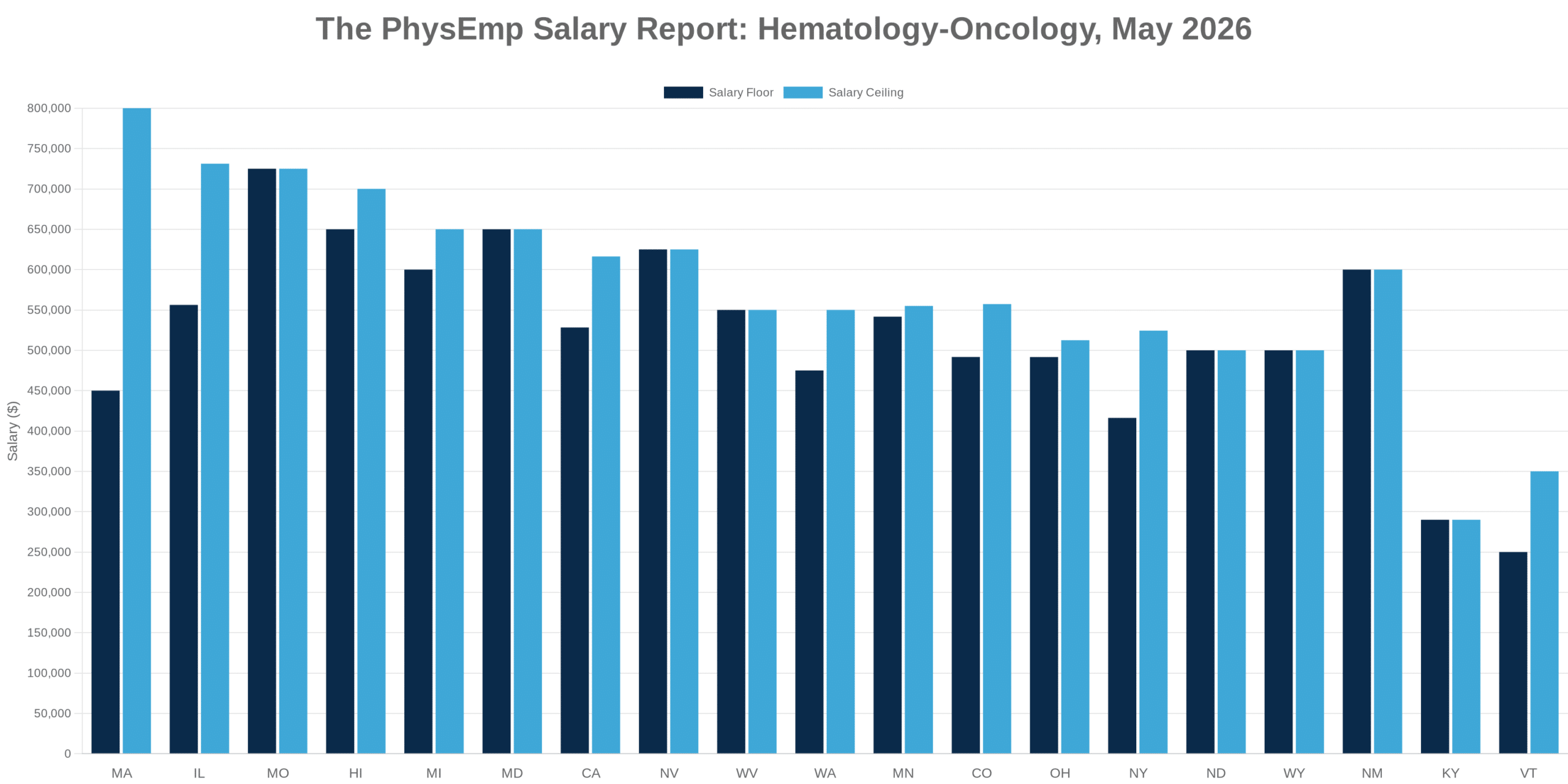This analysis synthesizes 6 sources published the week ending May 4, 2026. Editorial analysis by the PhysEmp Editorial Team.
The productivity metric that defines most physician compensation in America is generating pay disparities that can exceed one million dollars over a career—and the structural flaws embedded in wRVU-based models are becoming impossible to ignore. As health systems continue relying on work Relative Value Units as the primary lever for physician pay, a growing body of evidence suggests these models systematically undervalue certain specialties, create compliance vulnerabilities, and may be accelerating physician dissatisfaction with medicine itself. For physicians navigating today’s labor market and executives designing compensation packages, understanding the mechanics behind these disparities is essential to Physician Compensation & Demand strategy.
The Structural Flaw Behind Million-Dollar Pay Gaps
The wRVU system was never designed to be a comprehensive compensation framework—it was created as a Medicare reimbursement methodology. Yet health systems have universally adopted it as the dominant metric for determining physician pay. This translation from reimbursement tool to compensation engine has created profound distortions. Physicians performing identical clinical work in different settings, or those whose specialties involve significant non-procedural cognitive labor, find themselves systematically disadvantaged by a metric that privileges procedure volume over care complexity.
The pay gap problem compounds over time. When early-career physicians accept positions with suboptimal wRVU structures or conversion factors, the differential doesn’t remain static—it accelerates. A physician earning $50,000 less annually than a peer performing comparable work will see that gap exceed $1 million over a 20-year career when accounting for lost investment returns and retirement contributions. This isn’t merely a negotiation failure; it reflects structural inequities in how different practice environments value the same clinical productivity.
The wRVU system’s migration from Medicare reimbursement methodology to universal compensation metric has created structural pay inequities that compound dramatically over physician careers—a transformation that was never intentional and remains poorly understood by most physicians entering contract negotiations.
Not All wRVUs Are Created Equal: The Compliance Dimension
Mainstream coverage of physician compensation often treats wRVUs as a standardized, objective measure of productivity. This framing misses a critical economic reality: the compliance requirements surrounding wRVU-based compensation are complex, and violations can fundamentally alter the value proposition of any compensation arrangement. Health systems using wRVU thresholds, bonuses, or conversion factors must navigate Stark Law and Anti-Kickback Statute requirements that constrain how productivity incentives can be structured.
The legal landscape creates a paradox. Compensation must be set at fair market value and cannot vary based on the volume or value of referrals—yet wRVU models are explicitly designed to reward volume. This tension means that not all wRVU arrangements offer equivalent protection or value to physicians. Contracts with aggressive productivity thresholds or conversion factors that exceed market benchmarks may expose both parties to regulatory risk, while more conservative structures may leave physicians feeling undercompensated relative to their actual output.
For physicians evaluating offers, the compliance dimension adds a layer of due diligence that extends beyond comparing raw compensation figures. A contract offering higher per-wRVU rates but structured in ways that create regulatory exposure may ultimately prove less valuable than a more modest arrangement with stronger legal foundations.
Specialty Stratification and the Five-Year Compensation Trajectory
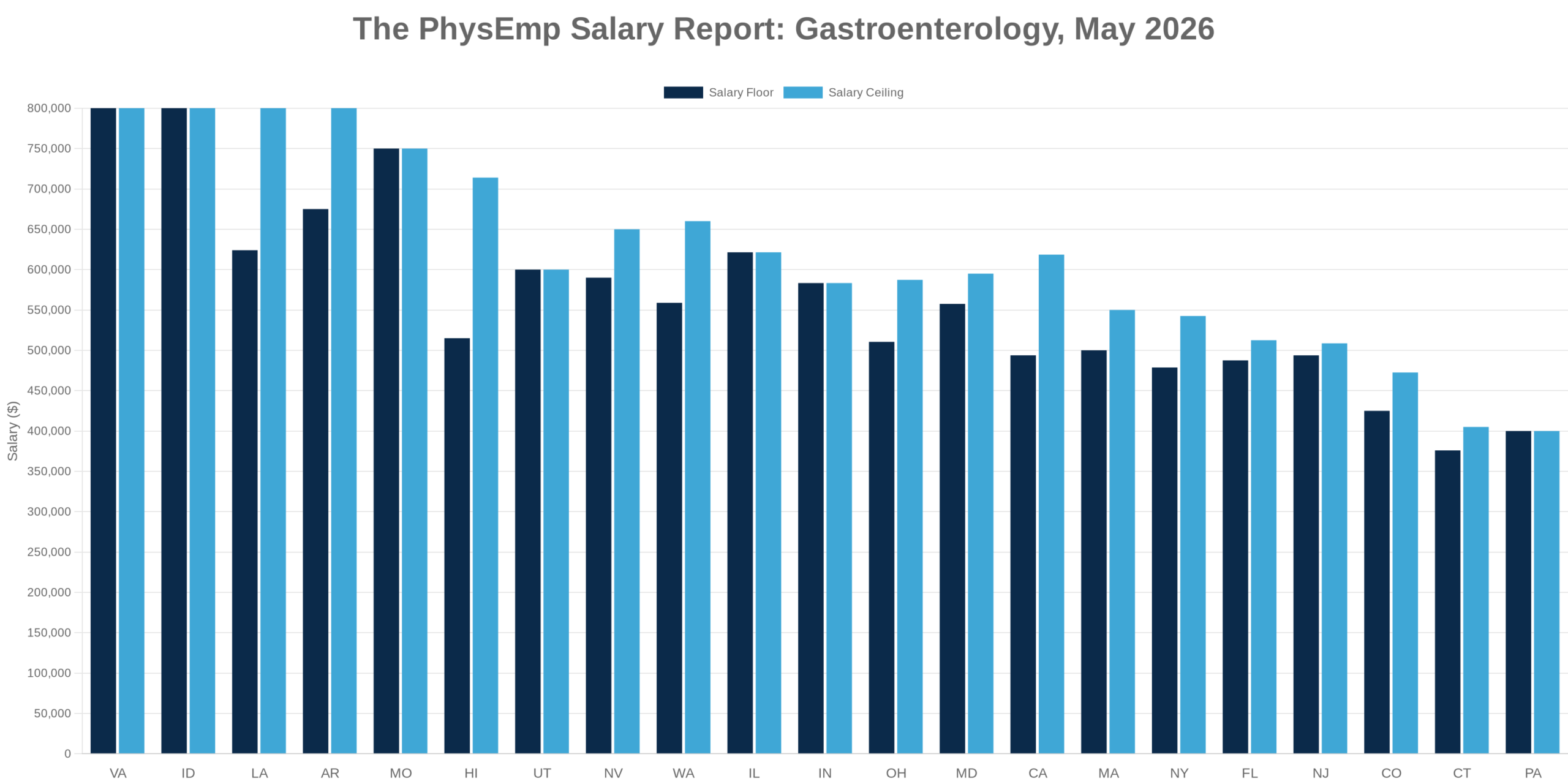
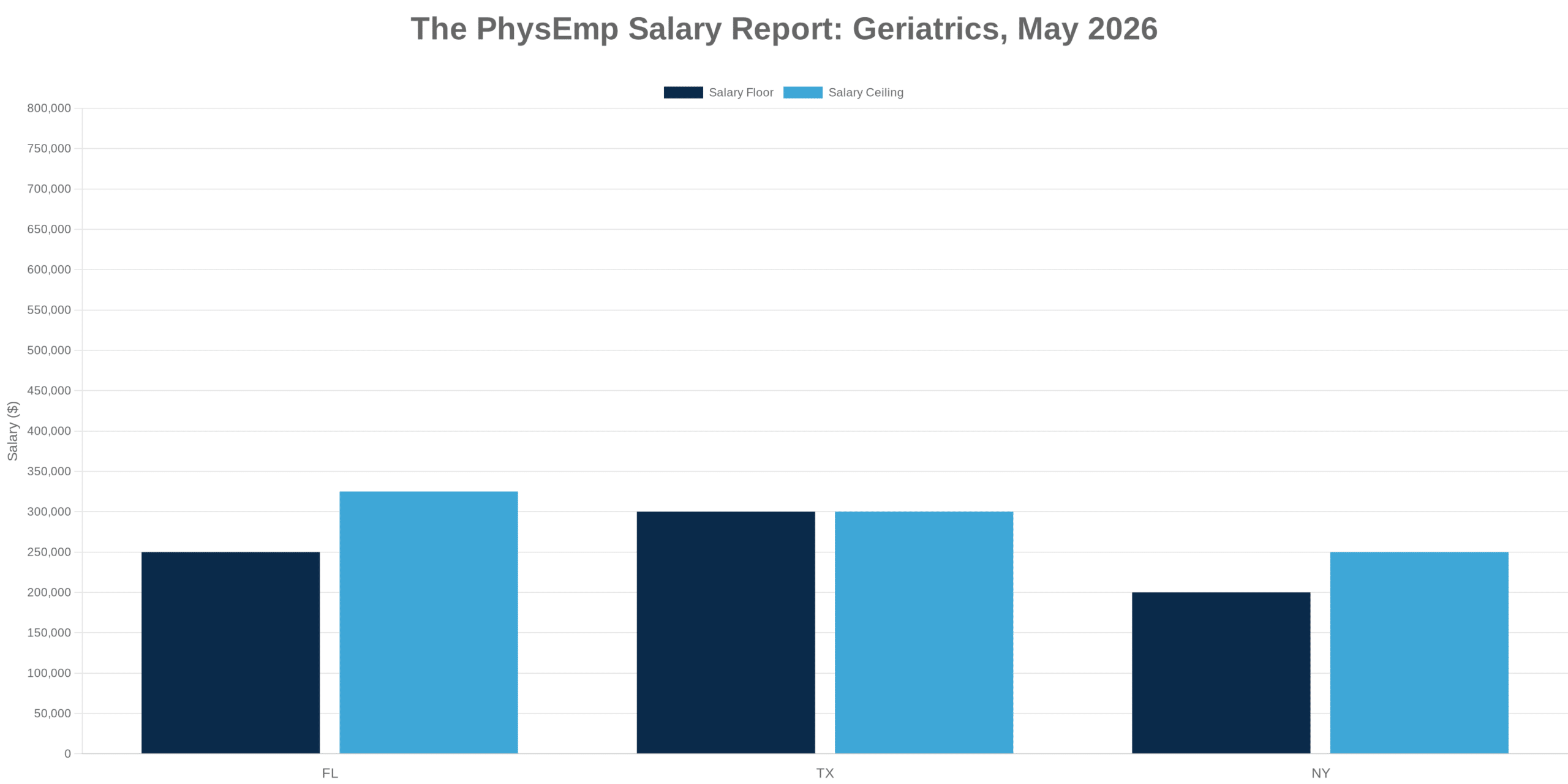
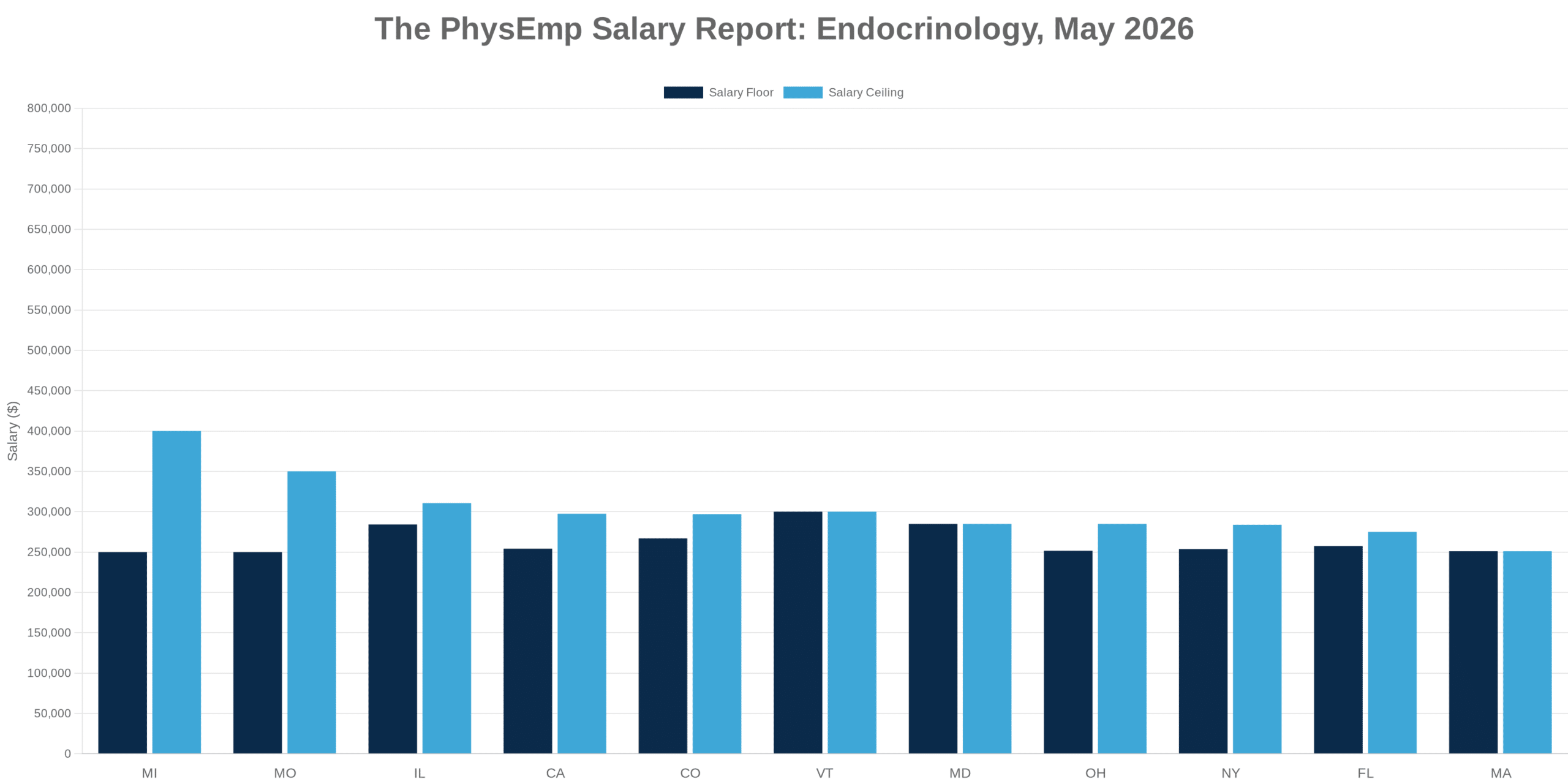
Analysis of the highest-paying physician specialties over the past five years reveals a consistent pattern: procedural specialties with high wRVU generation capacity dominate the top compensation tiers, while cognitive specialties and those involving substantial non-billable patient interaction lag significantly. This stratification isn’t news to anyone in healthcare, but the persistence and magnitude of these gaps deserve closer examination.
The specialties commanding premium compensation—typically surgical subspecialties and interventional fields—benefit from wRVU structures that capture their work relatively completely. A surgeon’s operating room time translates directly into billable units. By contrast, primary care physicians, psychiatrists, and others whose value includes care coordination, patient education, and longitudinal relationship management find much of their work invisible to the wRVU framework.
Hospital executives and recruiters face a strategic dilemma. The specialties most essential to population health management and value-based care success are often those most disadvantaged by wRVU compensation models. Recruiting and retaining primary care physicians, hospitalists, and behavioral health specialists requires either accepting compensation structures that may appear inflated relative to wRVU production or developing hybrid models that supplement productivity pay with alternative value metrics.
Health systems pursuing value-based care strategies while maintaining wRVU-dominant compensation models are working at cross-purposes—the physicians most critical to population health success are precisely those whose contributions the wRVU system fails to capture.
The Satisfaction Crisis as a Compensation Signal
When more than half of physicians express uncertainty about whether medicine is worth the investment, compensation structures deserve scrutiny as a contributing factor. The 53% figure reflecting physician ambivalence about their career choice cannot be attributed solely to administrative burden or work-life balance concerns—economic dissatisfaction plays a significant role, particularly when physicians perceive their compensation as disconnected from their actual value contribution.
The wRVU model exacerbates this disconnect. Physicians who entered medicine to provide comprehensive patient care find themselves evaluated and compensated based on a narrow slice of their professional activity. The resulting cognitive dissonance—working harder on dimensions that don’t translate to compensation while feeling pressure to optimize for metrics that may not align with patient needs—contributes to the broader satisfaction crisis.
For health systems, physician dissatisfaction has direct financial implications. Turnover costs for physicians typically range from $500,000 to over $1 million per departure when accounting for recruitment, onboarding, lost revenue during vacancy periods, and productivity ramp-up time. Compensation models that systematically generate dissatisfaction among certain physician populations represent a structural cost that rarely appears in compensation benchmarking analyses.
Strategic Implications for Compensation Design
The evidence points toward a compensation landscape in transition. Pure wRVU models, while offering apparent objectivity and administrative simplicity, carry hidden costs in the form of pay inequity, compliance complexity, specialty stratification, and physician dissatisfaction. Health systems and physician groups seeking competitive positioning must consider whether alternative or hybrid models might better serve their strategic objectives.
Physicians entering negotiations should approach wRVU-based offers with sophisticated analysis rather than simple benchmark comparison. Understanding how a proposed conversion factor compares to market rates matters, but so does evaluating the completeness of wRVU capture for their specific practice pattern, the compliance posture of the arrangement, and the long-term trajectory implications of accepting a particular structure.
The million-dollar pay gap is not inevitable—it results from structural choices that can be addressed through more thoughtful compensation design. As physician supply constraints intensify and competition for talent increases, organizations that develop compensation models reflecting the full spectrum of physician value contribution will hold meaningful advantages in recruitment and retention. The wRVU system served a purpose in its original Medicare context; its limitations as a universal compensation framework are becoming increasingly difficult to defend.
Sources
Physicians’ million-dollar pay gap problem – Becker’s ASC Review
Physicians’ million-dollar pay gap problem – Becker’s Hospital Review
Physicians’ wRVU problem by the numbers – Becker’s ASC Review
Health Care Law Today Episode 38: Let’s Talk Compliance — Not All wRVUs Are Created Equal – The National Law Review
10 highest-paying physician specialties in the last 5 years – Becker’s ASC Review
53% of Doctors Aren’t Sure Medicine Is Worth It – Medical Economics