This analysis synthesizes 8 sources published the week ending Apr 6, 2026. Editorial analysis by the PhysEmp Editorial Team.
Physician compensation is fracturing along multiple axes simultaneously—by specialty, by gender, by practice ownership structure, and by reimbursement model—creating a landscape where strategic positioning matters more than ever for earnings optimization. The convergence of stagnant Medicare reimbursement proposals, widening gender pay gaps in procedural specialties, and evolving compensation model structures signals a fundamental restructuring of how physicians are paid and who captures value in the current market. For physicians navigating career decisions and employers competing for talent, understanding these intersecting pressures is essential to Physician Compensation & Demand strategy.
Five-Year Specialty Compensation Trajectories Reveal Divergent Paths
Analysis of specialty compensation trends over the past five years reveals that not all physicians have experienced equal wage growth—and some have seen effective purchasing power decline when adjusted for inflation. The divergence between high-growth specialties and those facing reimbursement compression creates strategic implications for physicians evaluating long-term career positioning and for employers calibrating competitive offers.
What mainstream coverage often misses is that headline compensation figures obscure the underlying structural shifts in how that compensation is earned. A specialty showing modest total pay growth may simultaneously be experiencing intensified productivity demands, meaning physicians are working harder for proportionally less. Conversely, specialties with strong compensation growth may be benefiting from favorable supply-demand dynamics that create sustainable leverage rather than temporary market anomalies.
Physicians evaluating specialty career paths should analyze not just current compensation levels but the trajectory slope and the structural factors driving it—supply constraints, procedural mix shifts, and payer reimbursement trends all determine whether today’s pay advantage persists or erodes.
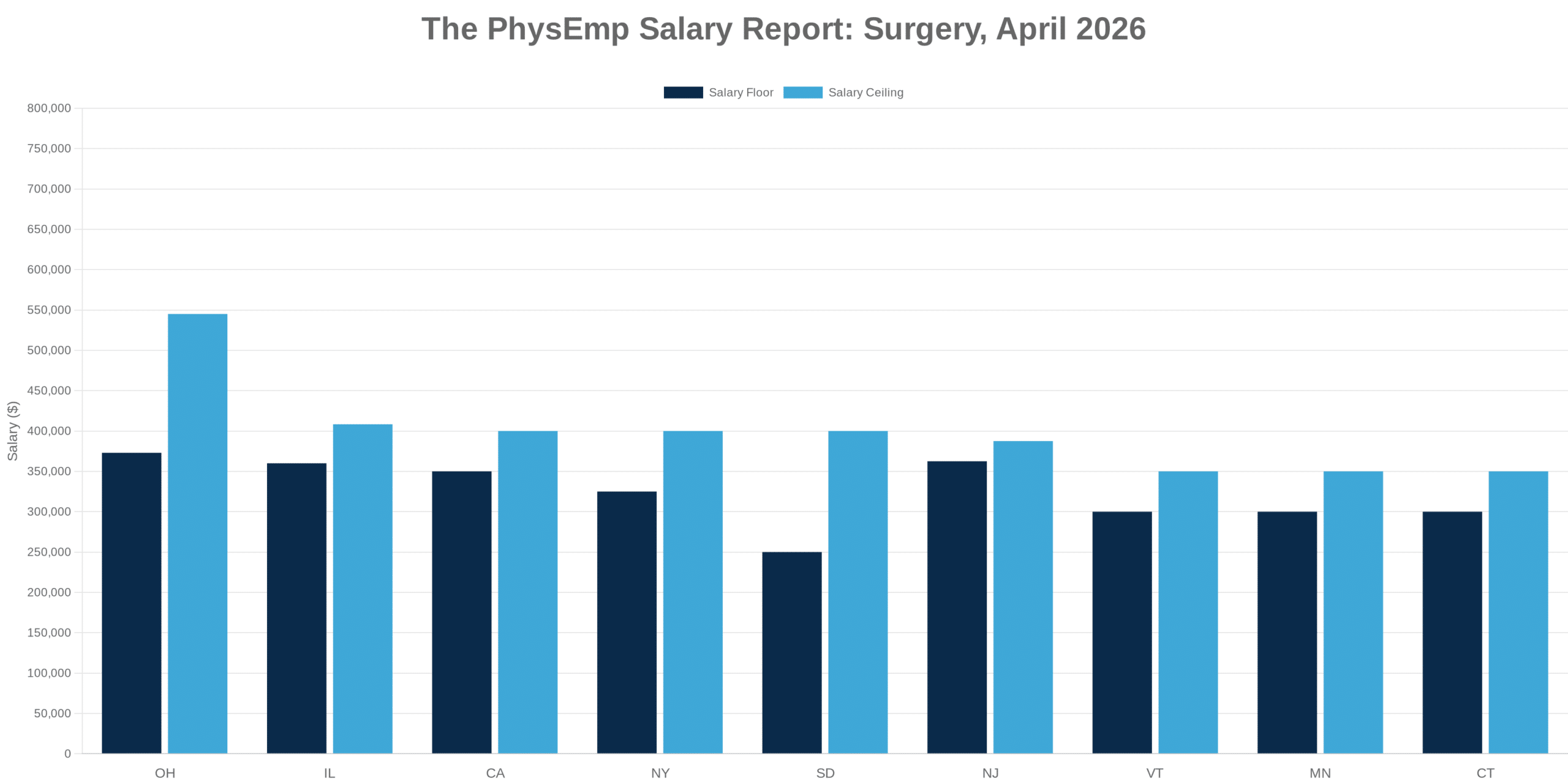
Surgeon Compensation Models Under Structural Review
The ongoing review of surgeon compensation models reflects broader tensions in how procedural specialists are paid. Traditional productivity-based models tied to RVUs face pressure from value-based care initiatives, while quality incentive components remain inconsistently implemented across health systems. Surgeons navigating contract negotiations must understand which compensation model elements are negotiable and which reflect systemic constraints their prospective employer cannot easily modify.
For hospital executives and practice administrators, the challenge lies in designing compensation structures that attract surgical talent while maintaining financial sustainability. The most competitive offers increasingly blend base salary guarantees with productivity upside and quality bonuses—but the weighting of these components varies significantly by market, specialty, and organizational strategy.
Practice Ownership Economics Reshape Income Composition
Data indicating that physician practice owners receive only 35% of income from salary illuminates the complex economics of practice ownership. The remaining income derives from practice profits, ancillary services, and other revenue streams that employed physicians typically do not access. This income composition difference has significant implications for total compensation comparisons between employed and owner-operator physicians.
For physicians evaluating employment versus ownership paths, the salary component alone provides an incomplete picture. Practice owners assume operational risk and administrative burden in exchange for potential upside that salaried positions cannot replicate. However, the consolidation trends reshaping healthcare delivery are compressing the opportunities for traditional practice ownership, potentially pushing more physicians toward employment models where salary represents a larger—but capped—share of total compensation.
Gender Pay Gaps in Ophthalmology Signal Broader Structural Issues
The documented million-dollar lifetime earnings gap for women in academic ophthalmology represents one of the starkest compensation disparities in medicine. This gap persists despite controlling for productivity metrics, suggesting that structural factors beyond individual performance drive the disparity. For a specialty with relatively balanced gender representation in training pipelines, the persistence of this gap raises questions about how compensation decisions are made and what systemic interventions might address the disparity.
The ophthalmology gender pay gap is not an isolated phenomenon but rather a particularly well-documented example of patterns that likely exist across multiple specialties. Physicians negotiating compensation—regardless of gender—benefit from understanding that initial offer anchoring, negotiation dynamics, and career trajectory decisions compound over time to create substantial lifetime earnings differences.
The million-dollar ophthalmology gender gap underscores that compensation negotiation is not a single event but a career-long process where early-career positioning decisions create compounding effects that persist for decades.
Medicare Reimbursement Policy Creates Systemic Uncertainty
The MedPAC recommendation for a 0.5% physician payment increase for 2027 continues a pattern of reimbursement adjustments that fail to keep pace with practice cost inflation. Legislative efforts to improve Medicare reimbursement stability acknowledge the problem but face uncertain political prospects. For physicians whose patient panels include significant Medicare populations, this reimbursement trajectory directly impacts earning potential and practice viability.
The policy uncertainty extends beyond Medicare itself. Commercial payers often benchmark to Medicare rates, meaning that Medicare reimbursement stagnation can cascade through the broader payer landscape. Physicians in specialties with high Medicare exposure face compounding pressure that their colleagues in specialties serving younger, commercially-insured populations may not experience as acutely.
Anesthesiology Compensation Transparency Shifts Market Dynamics
The viral response to an anesthesiologist’s twelve-year salary disclosure reflects growing interest in compensation transparency across medicine. As more physicians share compensation data publicly, information asymmetries that historically favored employers in negotiations are eroding. This transparency trend has implications for both physician negotiating leverage and employer recruiting strategies.
Health systems and practice groups that have relied on information advantages to constrain compensation offers may find that strategy increasingly ineffective. Conversely, organizations offering genuinely competitive compensation can leverage transparency to differentiate themselves in recruiting. The market is moving toward a more efficient pricing of physician labor—a shift that benefits well-informed physicians and transparent employers while disadvantaging those who relied on opacity.
Strategic Implications for Compensation Positioning
The convergence of specialty-specific trends, structural pay gaps, ownership economics, and reimbursement policy uncertainty creates a complex environment for compensation strategy. Physicians evaluating offers must look beyond headline salary figures to understand total compensation composition, productivity expectations, and the sustainability of current pay levels given reimbursement trajectories. Contract structures that appear favorable today may prove problematic if underlying reimbursement assumptions shift.
For employers, competitive positioning requires understanding not just current market rates but the directional pressures shaping physician expectations. Recruiting strategies that worked in an information-scarce environment may fail as transparency increases. The most successful organizations will be those that align compensation structures with physician priorities while maintaining financial sustainability—a balance that requires sophisticated analysis of specialty-specific dynamics and market-level supply-demand conditions.
Looking ahead, the physicians and organizations that thrive will be those who treat compensation not as a static negotiation outcome but as a dynamic strategic variable requiring ongoing attention to structural shifts, policy developments, and market evolution.
Sources
How 5 specialties’ pay has changed over 5 years – Becker’s ASC Review
Surgeon Compensation Models Reviewed – Conexiant
MedPAC: Increase physician pay by 0.5% for 2027 – Medical Economics
Murphy Introduces Legislation to Improve Medicare Reimbursement Stability – Office of Congressman Chris Murphy
Million-Dollar Earnings Gap for Women in Academic Ophthalmology – Medscape
Equal pay in ophthalmology? Not yet – Conexiant
Physician practice owners receive 35% of income from salary: AMA – Becker’s ASC Review
Anesthesiologist shares salary over 12 years — ‘not ready for the response’ – MSN