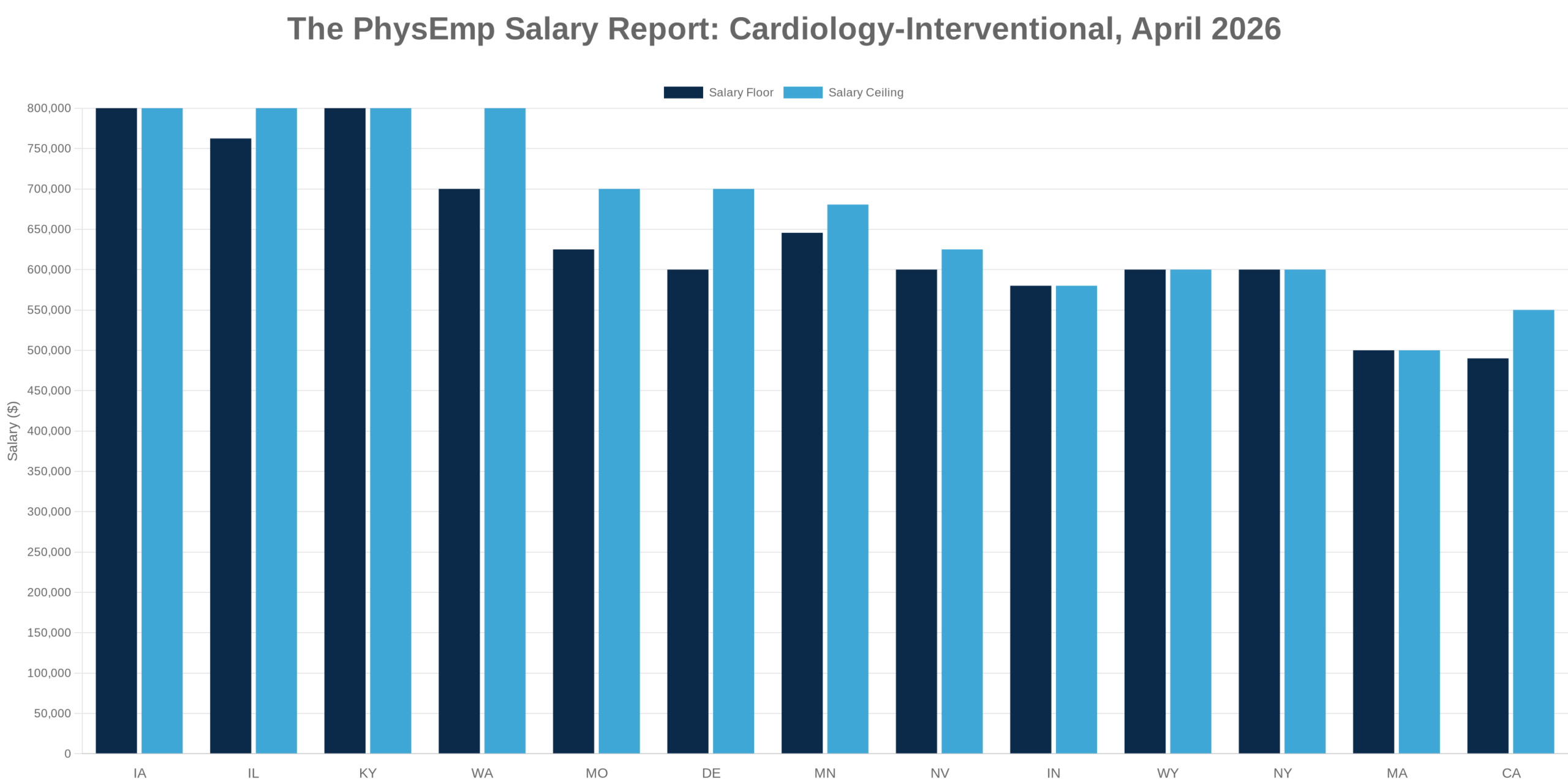
This analysis synthesizes 10 sources published the week ending Apr 8, 2026. Editorial analysis by the PhysEmp Editorial Team.
The physician shortage narrative in American healthcare has long centered on training pipelines—expanding residency slots, building new medical schools, and importing international graduates. But a growing body of evidence suggests this framing fundamentally misdiagnoses the problem. With 43.5% of family physicians now reporting burnout and turnover intentions climbing across specialties, the crisis isn’t about producing enough doctors—it’s about keeping the ones we have. This structural retention failure is reshaping the Healthcare Workforce & Labor Market in ways that traditional supply-side interventions cannot address.
The implications extend far beyond individual physician well-being. When experienced clinicians exit medicine prematurely—whether through early retirement, career pivots, or reduced clinical hours—healthcare systems lose not just headcount but accumulated expertise, patient relationships, and institutional knowledge that no residency expansion can quickly replace. The economic calculus of workforce planning must now account for a retention denominator that is actively shrinking.
The Burnout-Turnover Nexus: Beyond Individual Resilience
Recent data from Weill Cornell and multiple healthcare publications reveal that burnout among family physicians has reached critical mass, with nearly half reporting symptoms that correlate strongly with turnover intent. This isn’t a marginal workforce stress indicator—it represents a structural threat to primary care capacity at a moment when demand for these services continues to climb.
Mainstream coverage of physician burnout often frames it as an individual wellness challenge, suggesting that meditation apps, resilience training, or better work-life boundaries might stem the tide. This interpretation fundamentally misreads the labor economics at play. Burnout is not a personal failing requiring individual solutions; it is a market signal indicating that working conditions have deteriorated below the threshold many physicians are willing to accept, particularly when alternative career options exist.
When 43% of a specialty reports burnout symptoms correlated with exit intent, the problem isn’t physician fragility—it’s a labor market repricing risk as clinicians reassess whether current compensation and conditions justify continued practice.
The financial dimensions compound the psychological ones. Multiple analyses point to the interaction between burnout, student debt loads, and compensation stagnation as creating a perfect storm for workforce attrition. Physicians who entered medicine expecting certain income trajectories and practice autonomy now find themselves in employment structures that deliver neither, while administrative burdens consume increasing portions of their clinical time.
Moral Distress and the Limits of Systemic Tolerance
Beyond conventional burnout metrics, emerging research highlights moral distress as a distinct driver of workforce instability. Physicians increasingly report being unable to provide care they believe patients need due to administrative barriers, insurance constraints, or resource limitations. This ethical friction creates a form of occupational injury that resilience training cannot remediate.
The concept of “structural immiseration” gaining traction in physician advocacy circles captures this dynamic more accurately than burnout alone. It describes a systematic degradation of professional conditions—autonomy erosion, administrative burden escalation, and decision-making authority transfer to non-clinical entities—that cumulatively drives physicians toward exit.
For hospital executives and recruiters, this reframing carries significant implications. Compensation alone may no longer serve as the primary lever for talent acquisition and retention. Physicians evaluating opportunities increasingly weigh practice environment factors—administrative support ratios, electronic health record burden, schedule control, and clinical autonomy—as heavily as salary figures. Systems that fail to address these structural conditions will find themselves in perpetual recruitment cycles, replacing departing physicians at significant cost while never achieving workforce stability.
The Pipeline Fallacy: Why Training Expansion Alone Cannot Solve Retention Deficits
America’s approach to physician shortage has historically emphasized supply-side solutions: expanding medical school enrollment, increasing residency positions, and streamlining visa pathways for international medical graduates. These interventions address genuine bottlenecks but miss a crucial mathematical reality—if retention rates decline faster than training output increases, net physician supply continues to contract.
Consider the economics: training a physician requires seven to fifteen years depending on specialty, represents hundreds of thousands of dollars in educational investment, and produces a clinician who may practice for three decades or more. When that physician exits medicine a decade early due to burnout, the system loses not just current capacity but decades of future service. No training pipeline expansion can compensate for systematic early attrition at scale.
Every physician who leaves practice prematurely represents a training investment loss that would require years to replace—making retention economics potentially more valuable than recruitment spending for workforce-constrained systems.
The radiology community’s push for $45 million in federal funding for physician burnout programs signals growing specialty-level recognition that workforce sustainability requires active intervention. Yet even well-funded wellness programs may prove insufficient if they address symptoms rather than structural causes. The question facing healthcare leadership is whether organizations can fundamentally restructure practice environments or whether burnout-driven attrition will become an accepted cost of current operational models.
Strategic Implications for Workforce Competition
For physicians navigating career decisions, the current environment creates both risks and opportunities. Systems experiencing high turnover may offer premium compensation to attract talent but deliver working conditions that perpetuate the cycle. Conversely, organizations investing in structural practice improvements—reduced administrative burden, enhanced clinical support, meaningful autonomy—may offer more sustainable career environments even at comparable or lower compensation levels.
The due diligence calculus for physician job seekers should now include retention metrics, physician satisfaction data, and concrete evidence of systemic wellness investments rather than just stated commitments. Turnover rates within departments, average physician tenure, and administrative support ratios provide more predictive value than recruitment marketing materials.
For healthcare executives, the retention crisis demands a fundamental reexamination of physician employment economics. The total cost of turnover—recruitment expenses, productivity losses during transitions, patient relationship disruption, and remaining staff burden increases—often exceeds the investment required to address root causes of attrition. Organizations that recognize retention as a strategic priority rather than an HR function may achieve sustainable competitive advantages in increasingly tight labor markets.
Forward Outlook: Retention as the New Workforce Battleground
The physician workforce crisis is entering a phase where retention economics will increasingly dominate strategic planning. Training pipeline expansions will continue but cannot deliver results for years, while attrition pressures operate in real-time. Healthcare systems that successfully address structural drivers of burnout and moral distress will differentiate themselves in physician recruitment, while those relying solely on compensation competition will face escalating costs and persistent instability.
The policy landscape may shift as specialty societies and advocacy organizations push for federal investment in burnout mitigation, but systemic change at the organizational level will likely prove more immediately impactful than top-down interventions. Physicians hold increasing leverage in a supply-constrained market, and that leverage will increasingly manifest not just in compensation negotiations but in demands for practice environment improvements that address the structural conditions driving colleagues toward exit.
America’s physician shortage is real, but its solution lies less in producing more doctors than in keeping the ones we have. Until healthcare leadership internalizes this distinction, workforce instability will remain a defining feature of the clinical labor market.
Sources
43.5% of family physicians report burnout as turnover risk rises – Becker’s Hospital Review
Look to AMA’s Joy in Medicine program as physician burnout remains high – Fierce Healthcare
Burnout Driving Family Doctors to Quit Medicine Study Finds – U.S. News
43% of family physicians report feelings of burnout Weill Cornell – Fierce Healthcare
Physicians’ Moral Distress Linked to Burnout and Workforce Stability – DocWire News
America’s doctor shortage isn’t a training problem — it’s a retention problem – Medical Daily
Burnout Finances and the Growing Physician Exodus – MDLinx
Beyond Physician Burnout and Understanding Structural Immiseration – KevinMD
Bedri Yusuf Makes the Case for Structural Approaches to Physician Burnout – StreetInsider
Radiology pushes $45M fund for federal physician burnout program – Radiology Business