This analysis synthesizes 14 sources published the week ending Mar 4, 2026. Editorial analysis by the PhysEmp Editorial Team.
The national nursing shortage has crossed a structural threshold that is now triggering coordinated, multi-billion-dollar responses across education, philanthropy, and federal policy—signaling that healthcare systems are preparing for a prolonged period of constrained clinical labor supply. This week’s convergence of new nursing program launches, landmark endowment gifts, simulation lab investments, and bipartisan congressional pushback against proposed student loan caps reveals an industry-wide recognition that incremental workforce interventions are no longer sufficient. For stakeholders tracking the Healthcare Workforce & Labor Market, these developments represent a critical inflection point: the nursing pipeline is being systematically rebuilt, but the timeline for meaningful supply relief extends well into the next decade.
Educational Infrastructure Expansion Accelerates
Across multiple states, institutions are racing to expand nursing education capacity through new degree programs, simulation facilities, and clinical training partnerships. Colorado State University announced its first joint nursing degree specifically designed to address statewide shortages, while California State University San Bernardino is launching a Doctor of Nursing Practice program to expand advanced practice capacity. Rockland Community College in New York has broken ground on a $3 million nursing simulation lab, and the University of Cincinnati is emphasizing hands-on clinical experience as a core differentiator amid intensifying competition for nursing students.
These investments are not isolated institutional decisions—they reflect a coordinated response to workforce projections that show deepening shortages ahead. North Carolina, for example, faces a nursing deficit expected to worsen significantly in coming years, with current supply already inadequate to meet demand. The Western Slope region of Colorado is experiencing acute shortages that have prompted providers to directly partner with educational institutions to expand training pipelines.
The geographic dispersion of these nursing education investments reveals a critical pattern: regions historically underserved by clinical training infrastructure are now receiving targeted capacity expansion, suggesting healthcare systems are attempting to address rural and community hospital staffing gaps that have proven resistant to traditional recruiting approaches.
Philanthropic Capital Enters the Workforce Equation
Major philanthropic commitments are now flowing directly into nursing workforce development at unprecedented scale. Indiana University Health and the Ferguson family announced a landmark gift specifically aimed at strengthening the state’s nursing workforce, while Kennesaw State’s Wellstar School of Nursing secured a $700,000 scholarship endowment. These gifts represent a strategic shift in healthcare philanthropy—from facility construction and research funding toward direct investment in human capital pipelines.
For hospital executives and health system leaders, this philanthropic activity carries significant implications. Systems that can attract endowment-backed scholarship programs gain a structural advantage in recruiting nursing students who will graduate with reduced debt burdens and stronger institutional loyalty. The competition for philanthropic nursing investments may become as strategically important as competition for clinical talent itself.
The Preceptor Bottleneck
Mainstream coverage of nursing education expansion typically focuses on enrollment capacity and facility investments while overlooking a critical constraint: preceptor availability. Clinical preceptors—experienced nurses who supervise students during hands-on training—represent a binding constraint on how quickly nursing programs can scale. As highlighted in industry analysis this week, preceptor capacity directly affects both recruiting and retention outcomes. Systems that invest in preceptor development and compensation create a multiplier effect: they train more nurses while simultaneously improving retention among experienced staff who take on mentorship roles.
This bottleneck explains why simulation lab investments, while valuable, cannot fully substitute for clinical placement capacity. The nursing pipeline is constrained not merely by classroom seats or simulation equipment, but by the availability of working nurses willing and able to train the next generation—a classic supply-side constraint that standard workforce reporting frequently misses.
Federal Policy Threatens Pipeline Economics
A proposed Department of Education reclassification of professional degree programs—including nursing—would impose stricter student loan caps that industry stakeholders warn could devastate nursing school enrollment. More than 150 lawmakers, led by a bipartisan coalition including Senators Merkley and Wicker, have formally opposed the changes, arguing they would threaten the nursing profession at precisely the moment when pipeline expansion is most critical.
Senator Fetterman separately expressed opposition to the professional degree reclassification, while healthcare providers and universities have urged the Education Department to reconsider which occupations face stiffer loan limits. The core concern: nursing students already face significant debt burdens, and further restricting access to graduate-level loans would disproportionately affect students pursuing advanced practice credentials—the very workforce segment needed to address primary care and specialty shortages.
The federal loan cap debate exposes a fundamental tension in healthcare workforce policy: educational financing rules designed for general professional degree programs fail to account for the public health implications of restricting access to clinical training pipelines already operating below demand.
Implications for Physician Workforce Dynamics
Physicians evaluating career moves should recognize that nursing pipeline constraints directly affect practice economics and care team composition. Practices and systems unable to staff adequate nursing support will face pressure to either reduce patient volumes or shift clinical tasks to physicians—eroding the efficiency gains that team-based care models were designed to deliver. Conversely, systems that successfully expand nursing capacity may offer physicians more sustainable workload structures and better support ratios.
For hospital executives and recruiters, the nursing shortage creates complex interdependencies with physician recruiting. Facilities struggling to maintain nursing staff face higher physician turnover as practice conditions deteriorate. The most sophisticated recruiting strategies will increasingly integrate nursing workforce stability as a physician retention factor—a connection that remains underappreciated in standard recruiting metrics.
The Faculty Shortage Compounds the Crisis
Connecticut’s experience illustrates a compounding dynamic that threatens to limit the effectiveness of pipeline investments: nursing schools themselves face faculty shortages that constrain their ability to expand enrollment. Universities cannot simply add classroom capacity or simulation equipment if they lack qualified instructors to teach nursing students. This creates a recursive problem—the nursing shortage limits the ability to train more nurses—that requires longer-term solutions including faculty salary adjustments and pathway programs for experienced nurses to transition into academic roles.
Health systems investing in nursing education partnerships should recognize that faculty pipeline development may be as strategically important as student scholarship funding. Institutions that help nursing schools recruit and retain faculty gain preferential access to graduates and influence over curriculum alignment with clinical practice needs.
Looking Ahead: A Decade of Constrained Supply
The scale and coordination of this week’s nursing workforce investments signal that healthcare industry leaders have accepted a structural reality: meaningful supply relief is years away, and the intervening period will require sustained investment, policy advocacy, and operational adaptation. The nursing programs launching today will not produce graduates for three to four years at minimum, and advanced practice programs require even longer timelines.
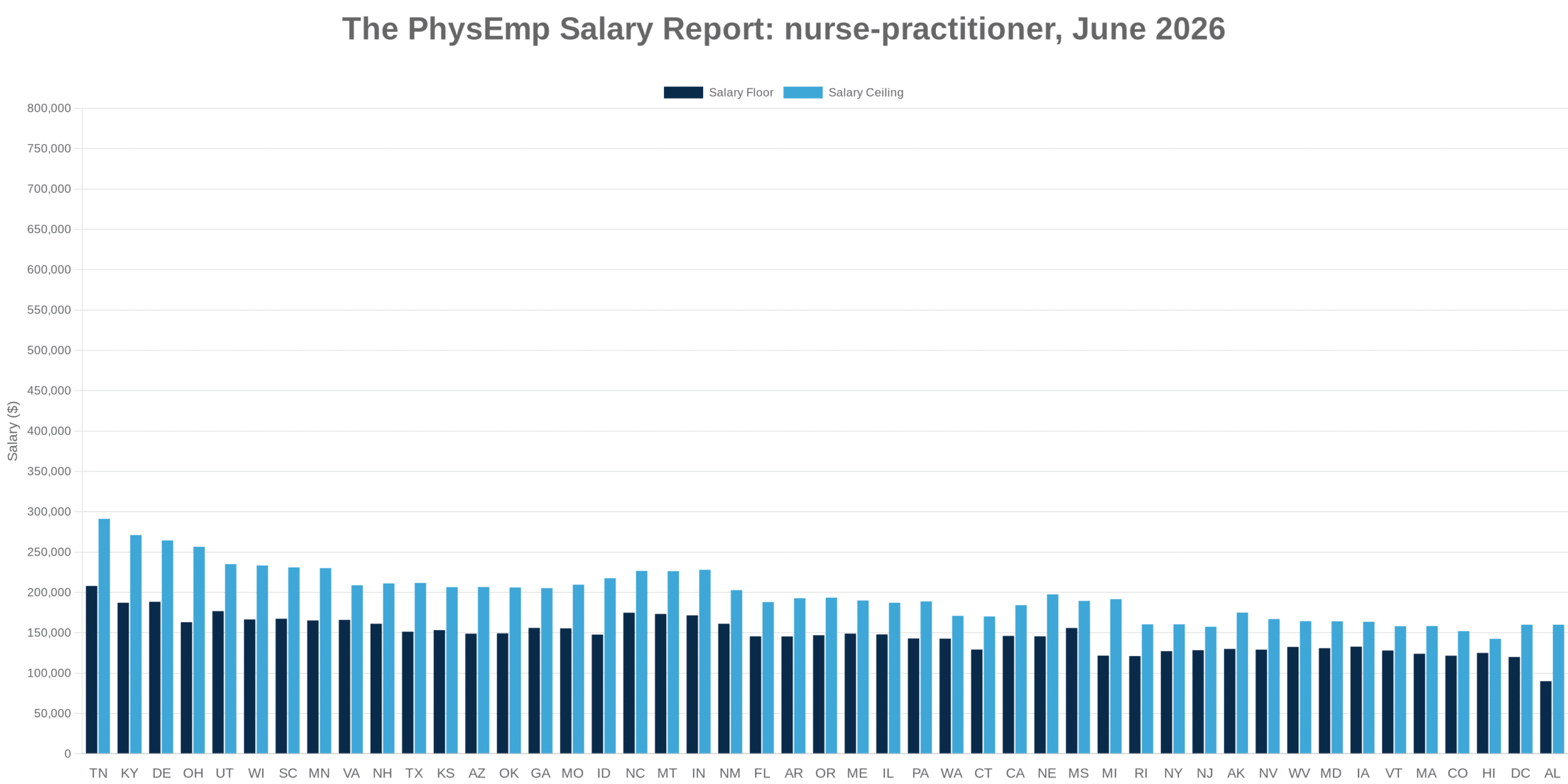
For healthcare labor markets, this extended timeline means continued upward pressure on nursing compensation, intensified competition for experienced nurses, and growing reliance on travel and contract staffing arrangements. Physicians and healthcare executives should plan for a decade in which nursing supply remains the binding constraint on care delivery capacity—shaping everything from facility expansion decisions to physician practice models to compensation structures across the clinical workforce.
Sources
CSU launching first joint nursing degree to tackle statewide nursing shortage – Denver7
Merkley Wicker Kiggans Bonamici & 150 Lawmakers: Changes to Nursing Student Loans Threaten the Profession – Office of Senator Jeff Merkley
Landmark gift from Connie and Steve Ferguson with IU Health investment to strengthen Indiana’s nursing workforce – WBIW
UC nursing students get hands-on experience amid national nursing shortage – WCPO
RCC starts construction of $3M nursing simulation lab – Westfair Online
In Letter to Department of Education Fetterman Expresses Opposition to Professional Degree Reclassification – U.S. Senator John Fetterman
North Carolina has a shortage of nurses. It’s expected to get a lot worse – Cardinal Pine
Connecticut’s nursing shortage leaves universities with less faculty – The Quinnipiac Chronicle
Colorado nursing shortage felt across Western Slope as providers look to expand training pipeline – Western Slope Now
HL Shorts: Why preceptors are key to nurse recruiting and retention – HealthLeaders Media
Providers urge Education Department to reconsider which jobs face stiffer student loan caps – Fierce Healthcare
Lawmakers and universities push back on loan caps – Inside Higher Ed
Kennesaw State’s Wellstar School of Nursing secures $700K scholarship endowment – Cobb County Courier
CSUSB to Launch Doctor of Nursing Practice Program – UKEN Report