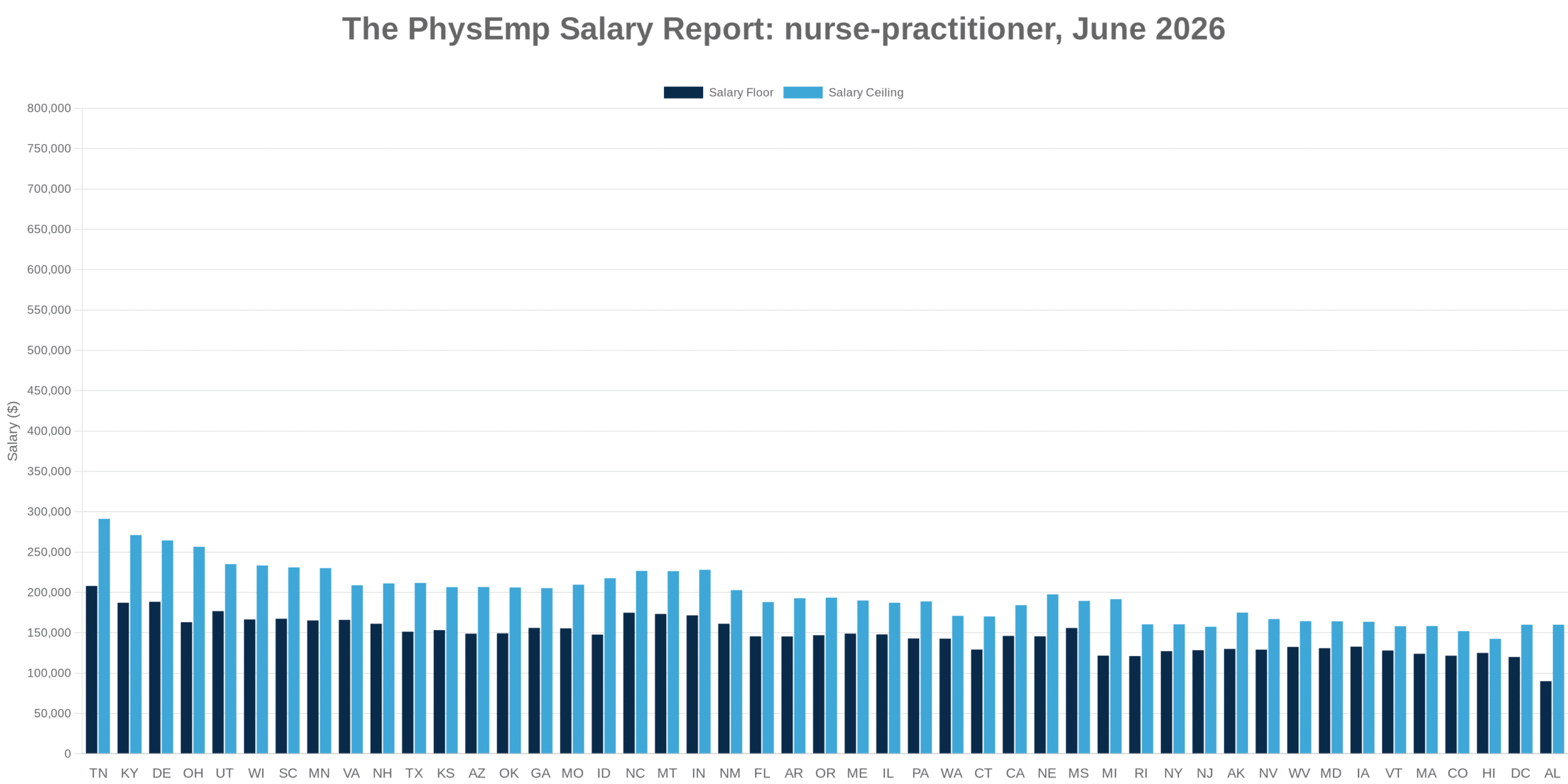
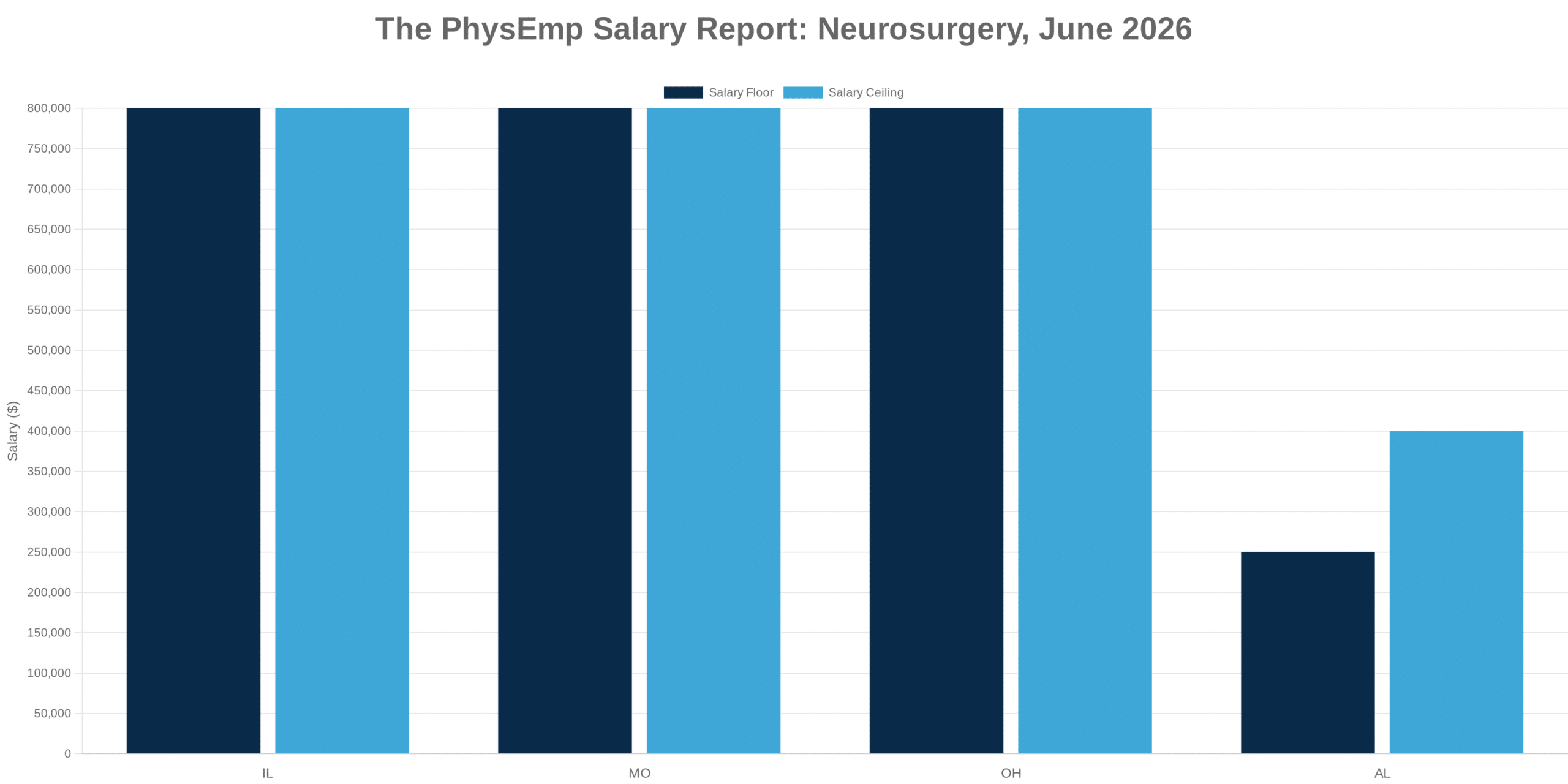
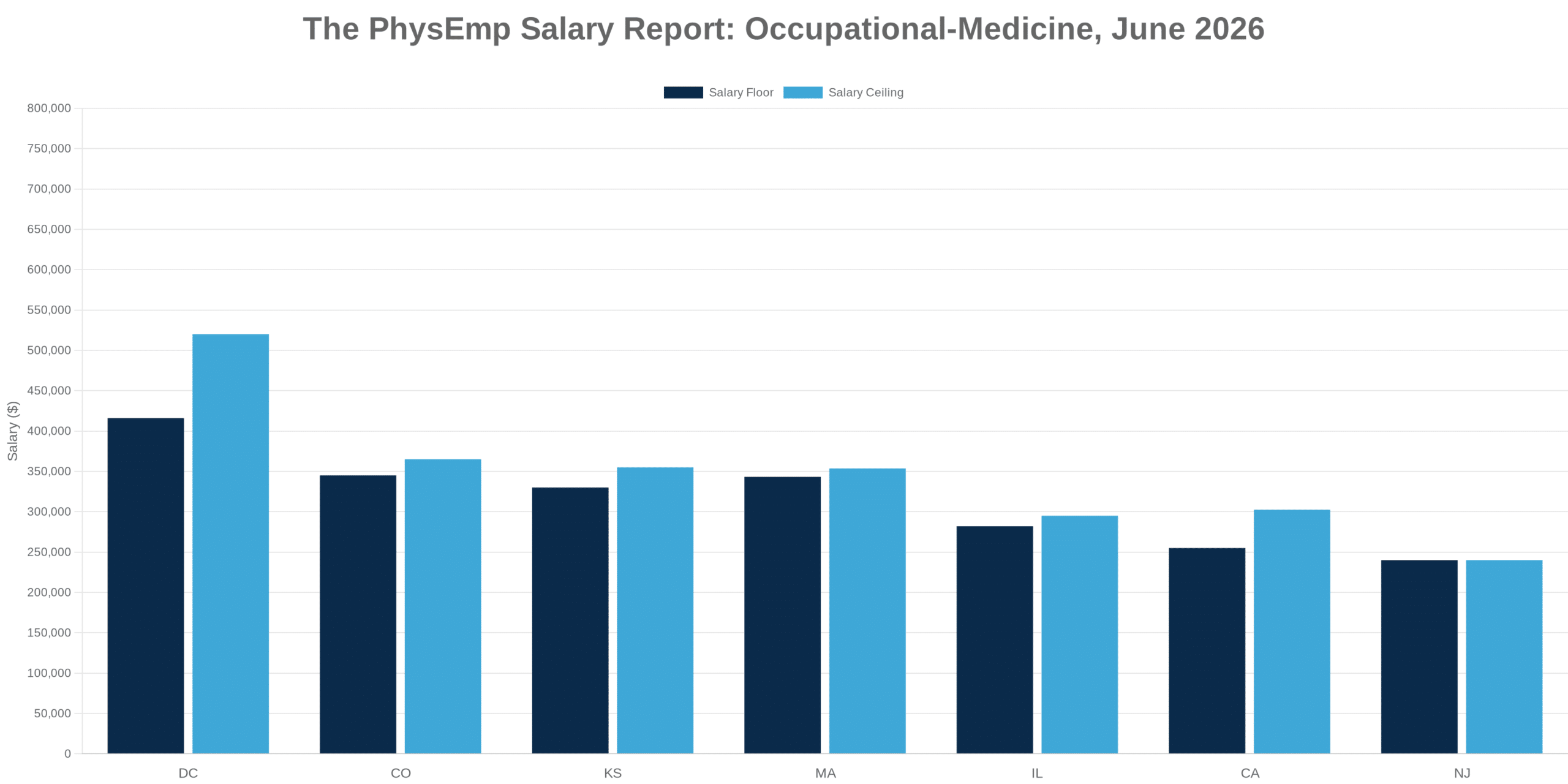
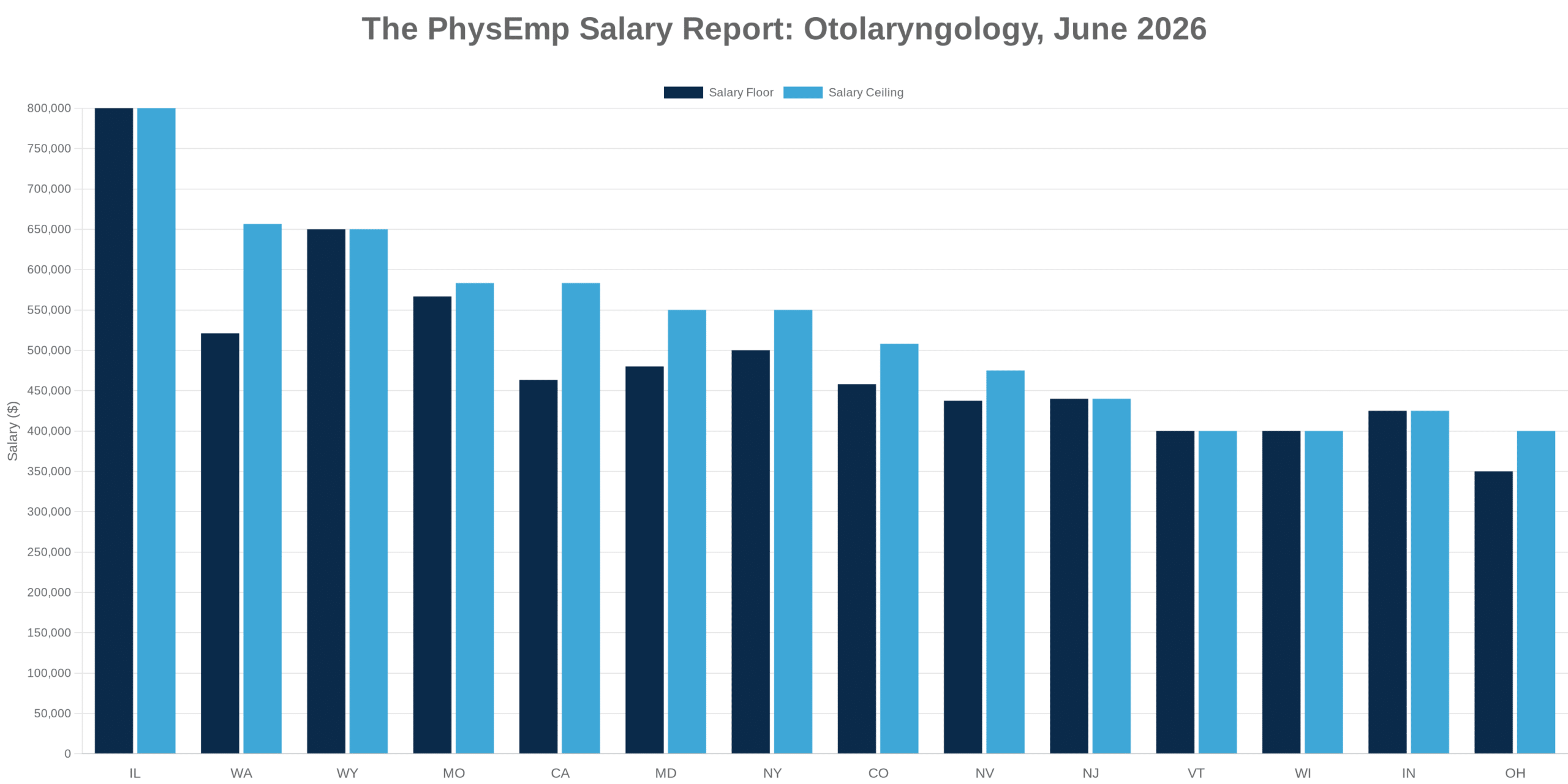This analysis synthesizes 8 sources published the week ending Mar 1, 2026. Editorial analysis by the PhysEmp Editorial Team.
Federal and state lawmakers are now engaged in a fragmented, often contradictory policy response to a nursing shortage that has reached structural crisis proportions. While bipartisan coalitions push for loan forgiveness expansions and educational pipeline investments, proposed federal caps on graduate student borrowing threaten to undermine the very nursing programs these initiatives aim to bolster. This tension reveals a fundamental disconnect in Healthcare Workforce & Labor Market policy—where workforce urgency collides with broader fiscal constraints, leaving health systems and clinical labor markets caught in regulatory crossfire.
The stakes extend well beyond nursing. As hospitals contend with RN vacancies that cascade into physician workload intensification, delayed care delivery, and constrained service lines, the policy battles unfolding in Washington and state capitals will shape clinical labor economics for the next decade. For physicians evaluating practice environments and health system executives competing for talent, understanding these legislative dynamics is essential to strategic workforce planning.
Federal Loan Policy: Pipeline Investment or Pipeline Threat?
The Department of Education’s proposed caps on graduate student borrowing have triggered bipartisan pushback from lawmakers who recognize the policy’s potential to devastate nursing education pipelines. Senator John Fetterman has emerged as a vocal critic, warning that limiting loan access for nursing students would exacerbate shortages precisely when workforce demand is accelerating. Senators Lisa Murkowski and Jeff Merkley have jointly urged the Department to consider exemptions for rural nursing programs, highlighting how borrowing restrictions would disproportionately impact training programs serving underserved regions.
Universities and higher education advocates have amplified these concerns, noting that nursing programs—particularly advanced practice and graduate-level tracks—rely heavily on federal student loan access. The proposed caps, designed to address broader concerns about graduate student debt burdens, fail to account for the distinct labor market dynamics of healthcare professions where demand vastly outstrips supply.
Federal loan policy designed for general graduate education markets creates unintended workforce consequences when applied to healthcare training pipelines. Nursing programs face a paradox: the same debt concerns driving policy reform are symptoms of inadequate public investment in clinical education infrastructure.
What mainstream coverage of this policy debate often misses is the downstream physician impact. Nursing shortages don’t exist in isolation—they create staffing gaps that intensify physician workloads, accelerate burnout, and constrain the care delivery models that health systems can sustain. When RN pipelines contract, the pressure redistributes across the entire clinical workforce, affecting physician practice economics and employment conditions in ways that loan policy debates rarely acknowledge.
State-Level Responses: Staffing Mandates and Scope Expansion
While federal policy debates stall, state legislatures are advancing competing strategies to address nursing shortages through regulatory intervention. Wisconsin’s proposed Nurse Staffing & Patient Protection Act represents one approach—mandating minimum nurse-to-patient ratios that proponents argue will improve retention by addressing workload concerns that drive RNs from bedside care. Missouri has taken a different tack, pursuing legislation that would expand nursing scope of practice and create educational partnerships to accelerate workforce entry.
These divergent state strategies reflect genuine uncertainty about whether the nursing shortage is primarily a supply problem (insufficient training capacity), a retention problem (poor working conditions driving exits), or a distribution problem (geographic maldistribution of available nurses). The evidence suggests all three dynamics are operating simultaneously, which explains why no single policy lever has proven sufficient.
For hospital executives and physician leaders, the state-level regulatory landscape creates operational complexity. Staffing mandates may improve nurse retention but constrain scheduling flexibility and increase labor costs. Scope expansion may address task distribution but raises questions about care team coordination and physician oversight responsibilities. Neither approach directly addresses the fundamental pipeline constraints that limit aggregate nursing supply.
Rural and Specialty Workforce Collapse
The nursing shortage’s geographic dimension has reached crisis intensity in rural markets, where workforce constraints are forcing service line closures that reshape regional healthcare access. Pennsylvania’s expanding “maternity deserts”—rural areas where obstetric services have become unavailable due to staffing and financial pressures—illustrate how nursing shortages compound with physician workforce gaps to create care delivery voids.
North Carolina projections indicate the state’s nursing shortage will worsen significantly in coming years, with rural and community hospitals facing the steepest declines. These forecasts reflect demographic realities: an aging nursing workforce approaching retirement, insufficient training program capacity to replace departing RNs, and competitive dynamics that pull new graduates toward urban health systems offering higher compensation and better working conditions.
Rural workforce collapse follows a predictable pattern: nursing shortages force service line closures, which reduce physician practice viability, which accelerates physician departures, which further constrains the care infrastructure that might attract replacement clinicians. Breaking this cycle requires coordinated intervention across multiple workforce categories.
For physicians in rural practice or considering rural opportunities, these dynamics carry direct career implications. Practice sustainability increasingly depends on nursing workforce stability—a factor largely outside individual physician control but central to employment security and professional satisfaction.
Retention Economics: What Would Bring Nurses Back?
Survey data on nursing workforce preferences reveals that compensation alone is insufficient to address retention challenges. RNs who have left hospital practice cite workload intensity, inadequate staffing, lack of professional autonomy, and burnout as primary drivers of their exit decisions. Bringing these nurses back requires structural changes to practice environments—changes that carry significant cost and operational implications for health systems.
This retention challenge intersects with physician workforce dynamics in important ways. Care delivery models that rely on team-based approaches require stable nursing complements to function effectively. When nursing turnover disrupts team continuity, physicians absorb additional coordination burdens and documentation responsibilities that compound their own burnout risks. The workforce crises in nursing and medicine are not parallel problems—they are interconnected pressures that amplify each other.
Health system executives competing for physician talent must recognize that nursing workforce stability is a physician recruitment asset. Candidates evaluating employment opportunities increasingly assess support staff adequacy as a factor in practice sustainability and quality of professional life. Systems that cannot demonstrate nursing workforce stability face competitive disadvantages in physician recruiting markets.
Strategic Implications for Workforce Planning
The current legislative landscape suggests that meaningful federal intervention on nursing workforce pipelines remains uncertain, with loan policy debates creating potential headwinds even as bipartisan coalitions advocate for expanded support. State-level responses will continue to vary, creating a patchwork regulatory environment that complicates multi-state health system workforce planning.
For physicians, these dynamics reinforce the importance of evaluating employer workforce stability when considering career moves. Practice environments with chronic nursing shortages carry elevated burnout risks and may face service line constraints that limit professional development opportunities. For health system leaders, the policy uncertainty argues for accelerated investment in internal training pipelines, retention-focused practice environment improvements, and compensation strategies that account for regional competitive dynamics.
The nursing shortage is not a temporary disruption awaiting policy resolution—it is a structural feature of healthcare labor markets that will shape clinical workforce economics for the foreseeable future. Strategic positioning requires acknowledging this reality and planning accordingly.
Sources
Fixing the nursing shortage: What would bring RNs back to hospitals? – DocWire News
Fetterman pushes back on federal plan affecting nursing student loans – Gant News
Lawmakers and universities push back on loan caps – Inside Higher Ed
Missouri bill looks to help nurses address health-care shortage – WGEM
North Carolina has a shortage of nurses. It’s expected to get a lot worse – Cardinal & Pine
Wisconsin Nurse Staffing & Patient Protection Act – Nurse.org
Murkowski, Merkley Send Letter Urging Department of Education to Help Address Rural Nursing Shortage – Office of U.S. Senator Lisa Murkowski
States’ maternity deserts are reaching a crisis point as rural hospitals continue to close childbirth services – City & State PA